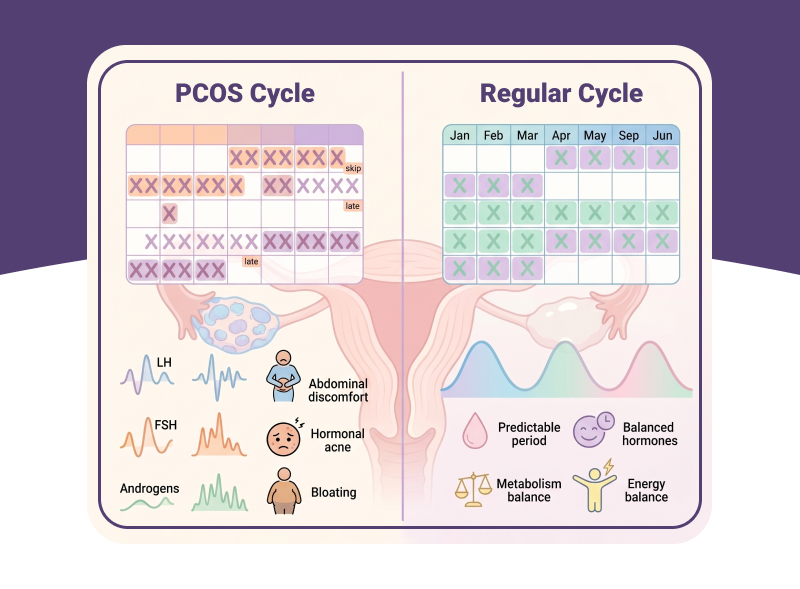
PCOS periods and regular periods can differ in timing, flow, and underlying hormone patterns. With polycystic ovary syndrome (PCOS), menstrual cycles may often be irregular, delayed, or sometimes absent, although some individuals may still experience bleeding that appears regular.
In comparison, regular periods typically follow a predictable cycle pattern (around 21–35 days) with relatively consistent ovulation and similar flow each month. Tracking ovulation and cycle patterns over time may help identify these differences more clearly.
Key Takeaways
- PCOS with regular periods may occur in some cases, and menstrual bleeding does not always indicate that ovulation has occurred.
- PCOS-related period symptoms may include heavier or less predictable flow, as well as symptoms associated with higher androgen levels.
- Having regular periods may not always reflect consistent ovulation, as cycles without ovulation can still happen.
- Tracking LH patterns may help predict ovulation, and basal body temperature (BBT) may help provide insight into whether ovulation has likely occurred.
- The easy@Home and Premom fertility system may help users observe subtle cycle irregularities over time.
Key Terms Explained
- Anovulation: A cycle where the ovaries fail to release an egg despite vaginal bleeding.
- Androgens: Male-type hormones, like testosterone, that are often elevated in PCOS.
- LH surge: A rise in luteinizing hormone that typically triggers the release of an egg within 24–36 hours.
- Polycystic ovary syndrome (PCOS): A hormonal condition characterized by irregular cycles, androgen excess, or polycystic ovaries.
- Basal body temperature (BBT): The body’s lowest resting temperature, which rises post-ovulation and may help indicate whether ovulation has likely occurred.
What Are PCOS Periods vs Regular Periods?
A normal menstrual cycle lasts between 21 and 35 days, with ovulation often occurring around the middle of the cycle. In contrast, periods with polycystic ovaries may be shorter than 21 days or longer than 35 days, with possible disruption in ovulation due to hormonal imbalances.
What Are Polycystic Ovaries Periods?
Polycystic ovary syndrome periods may be linked to what is sometimes described as an “ovulatory standoff,” where the body may attempt to ovulate but does not complete the process. This may contribute to unpredictable cycles or irregular menstruation. According to NCBI, ovulatory dysfunction is a core feature of PCOS, and the condition is estimated to account for approximately 80% of anovulatory infertility cases, indicating that many women with PCOS may experience irregular or disrupted cycles.
How a Normal Menstrual Cycle Works
A healthy cycle involves a precise rise and fall of estrogen and progesterone. This process ensures the uterine lining grows and sheds predictably after an egg is released.
Can You Have PCOS with Regular Periods?
Yes, it may be possible to have PCOS even with regular menstrual cycles. This pattern is sometimes referred to as “ovulatory PCOS,” where regular bleeding occurs, but other diagnostic features — such as elevated androgen levels or polycystic ovarian morphology on ultrasound — may still be present. In some cases, regular cycles may not always reflect consistent ovulation or optimal fertility patterns.
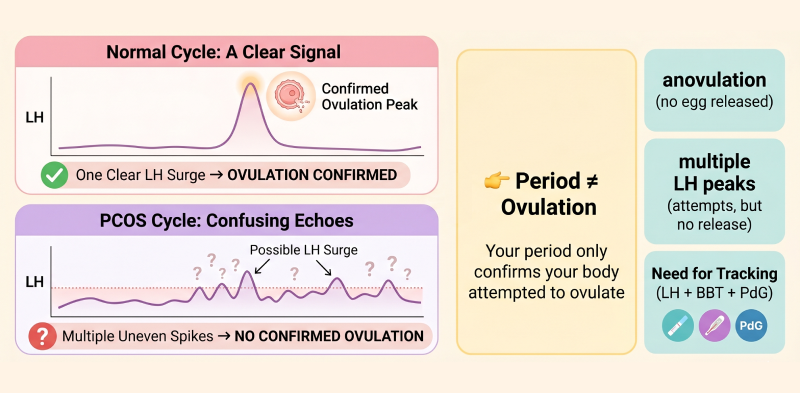
Why Regular Bleeding Doesn’t Always Mean Ovulation
Bleeding can occur without an egg being released. This is known as “estrogen withdrawal bleeding.” In these cases, the body sheds the uterine lining even though ovulation has not occurred. Because of this, some individuals with PCOS may have cycles that appear regular on a calendar but may still be experiencing anovulatory cycles.
Signs You May Still Have PCOS
Even with regular periods, other symptoms may still be present. These can include adult acne, thinning scalp hair, or excess hair growth on the face or body. If any of these signs are familiar, speaking with a healthcare provider may be a helpful next step.
PCOS Period Symptoms vs Regular Period Symptoms
Comparing PCOS period symptoms to a standard cycle reveals differences in flow and physical discomfort.
| Feature | PCOS Periods | Regular Period |
|---|---|---|
| Cycle Timing | May appear regular but inconsistent | Predictable (21–35 days) |
| Ovulation | Often irregular or absent | Often occurs consistently |
| Flow | Heavy or unpredictable | Moderate, consistent |
| Pain | Mild to moderate cramps; one-sided (unilateral) cramping may occur due to cystic ovaries | Mild to moderate cramps |
| Hormones | Elevated androgens, insulin resistance | Balanced hormones |
| Fertility Impact | May be more difficult to identify fertile timing without tracking | More predictable timing if ovulating regularly |
Regular Periods vs Ovulation: What’s the Difference?
Having a regular period does not always mean that ovulation is occurring consistently. Some cycles may involve bleeding without the release of an egg, especially in conditions like PCOS. Tracking hormone patterns and ovulation signals may help provide a clearer understanding of whether a cycle is ovulatory.
PCOS Pain vs Normal Period Pain
For some individuals, period-related discomfort with PCOS may feel more intense or persistent than in a typical cycle. This can include pelvic pressure, bloating, or cramping that lasts longer or occurs outside of the expected period window. However, pain experiences can vary from person to person.
What Does a PCOS Flare Feel Like?
A PCOS flare-up may involve sudden pelvic pressure, bloating, and intense cramping sensations. These flares may be influenced by factors such as high sugar intake or increased stress levels.
Are PCOS Cramps Different from Typical Period Cramps?
In polycystic ovary syndrome, cramping isn’t necessarily more severe, but it may feel different. Some people notice pelvic discomfort that can occur during or between periods, and occasionally on one side, depending on ovarian activity.
How to Know If You Have PCOS with Regular Periods
If you’re wondering whether PCOS is possible even with regular cycles, it may help to look beyond just the calendar pattern. Healthcare providers often refer to the Rotterdam Criteria, where a diagnosis may be considered if at least two of the following are present: irregular or absent ovulation, signs of elevated androgens, or polycystic ovarian morphology on ultrasound.
Key Diagnostic Signs Beyond Cycles
Even when periods appear regular, some individuals may still show features associated with PCOS. Blood tests may indicate higher androgen levels, and in some cases, an altered LH to FSH ratio may be observed. These findings, along with clinical symptoms such as acne, hair thinning, or excess hair growth, may suggest underlying hormonal imbalance and metabolic changes.
How Tracking Improves Conception
Using tools like easy@Home ovulation tests along with the Premom app may help you observe LH patterns across your cycle. Tracking these trends and pairing them with other signals like basal body temperature may provide better insight into whether a cycle is likely ovulatory and help guide timing for conception.
How to Track Ovulation Accurately with PCOS
Even if your periods appear regular, tracking ovulation with PCOS may require more than just counting days. Because ovulation may not occur consistently, using multiple signals can help you better understand what’s happening in each cycle.
Step 1: Log Your Period Start Date
Use the Premom ovulation tracker app to record the first day of your period in each cycle. Over time, this information may help you observe patterns and better understand your cycle length and variability.
Step 2: Start Testing After Your Period Ends
Begin using easy@Home ovulation test strips daily after your period. Testing once or twice a day may help capture LH changes, especially in irregular cycles.
Step 3: Check Cervical Mucus
Look for clear, stretchy, slippery mucus similar to raw egg whites, which may suggest that your fertile window is approaching.
Step 4: Log Results Consistently
Upload your test strips in the Premom app to track numerical LH values and view trends over time rather than relying on a single result.
Step 5: Look for Your LH Rise
Focus on identifying your highest LH level compared to your usual baseline, rather than relying on a single positive result. In PCOS, LH levels may be elevated throughout the cycle, so trends over time may be more meaningful.
Step 6: Add BBT Tracking
Measure your basal body temperature each morning before getting out of bed. A sustained rise in temperature over a few days may suggest that ovulation has likely occurred.
Step 7: Track PdG After the Surge
Using PdG test strips in the days following a suspected LH peak may provide additional context about progesterone levels, helping to further indicate whether ovulation has occurred.
Step 8: Review Patterns Across Cycles
Tracking over multiple cycles may help you better understand your personal ovulation patterns and whether ovulation is occurring consistently, even if your periods appear regular.
Track Your Cycle Health with Premom
Understanding your cycle patterns with polycystic ovary syndrome may be a helpful first step toward gaining more clarity about your health. Use the easy@Home and Premom fertility system to track your LH levels and identify your unique patterns. Pair your tracking with PCOS Pro to receive deeper insights into your PCOS period symptoms and hormonal trends.
PCOS Pro is a 6-month access pass inside the Premom app, built specifically for people with irregular cycles or PCOS. It unlocks additional tracking tools and educational resources focused on deeper cycle awareness.
What PCOS Pro includes:
- Tracking tools designed for irregular or unpredictable cycles
- Daily health logs for sleep, nutrition, and stress patterns
- Cycle insights that build as more data is collected
- Educational guidance focused on PCOS and hormone health
Tracking these signals together may help users gain a clearer understanding of their cycle patterns over time.
Frequently Asked Questions About PCOS Periods
It may be possible to have PCOS with regular menstruation. In such cases, other features like elevated androgen levels or polycystic ovarian morphology may be considered during evaluation rather than cycle length alone.
Some individuals with PCOS may experience more intense symptoms, which could include heavier bleeding or stronger cramps compared to what is typically expected in a cycle, though experiences can vary.
Periods with Polycystic Ovary Syndrome don’t follow a single pattern. Cycles may be irregular, less predictable, or sometimes heavier when they do occur. The overall experience can vary significantly, so no one set of symptoms defines a “PCOS period.”
The term “PCOS belly” is sometimes used to describe fat distribution around the abdominal area, which may be linked to metabolic factors such as insulin resistance commonly associated with polycystic ovary syndrome.
Disclaimer: Premom provides educational information and tracking tools. It is not medical advice. For medical guidance, consult a healthcare professional. Premom’s Ask AI is purely informational and educational and is not a substitute for professional medical advice, diagnosis, or treatment of any kind.
References
- Wolf WM, Wattick RA, Kinkade ON, Olfert MD. Geographical Prevalence of Polycystic Ovary Syndrome as Determined by Region and Race/Ethnicity. Int J Environ Res Public Health. 2018;15(11):2589. doi:10.3390/ijerph15112589 https://pmc.ncbi.nlm.nih.gov/articles/PMC6266413/
- McCartney CR, Marshall JC. Polycystic Ovary Syndrome. N Engl J Med. 2016;375(1):54–64. doi:10.1056/NEJMcp1514916 https://pubmed.ncbi.nlm.nih.gov/27406348/
- Teede HJ, Misso ML, Costello MF, et al. Recommendations from the international evidence-based guideline for the assessment and management of polycystic ovary syndrome. Fertil Steril. 2018;110(3):364–379. doi:10.1016/j.fertnstert.2018.05.004 https://pubmed.ncbi.nlm.nih.gov/30033227/
- Melo AS, Ferriani RA, Navarro PA. Treatment of infertility in women with polycystic ovary syndrome: approach to clinical practice. Clinics (Sao Paulo). 2015;70(11):765–769. doi:10.6061/clinics/2015(11)09 https://pmc.ncbi.nlm.nih.gov/articles/PMC4642490/