An ovulation tracking app for PCOS helps you track hormone patterns, irregular cycles, and ovulation signals over time. By combining ovulation tests, temperature tracking, and symptom logging, it may help you better understand your cycle and identify potential fertile windows — especially when cycles are unpredictable. This may all be helpful when trying to get pregnant with PCOS.
A structured 6-month tracking approach that includes ovulation tests, cycle logging, and symptom monitoring may provide insights into hormone patterns and possible fertile windows over time.
Using an ovulation tracking app may help individuals with polycystic ovary syndrome interpret irregular cycle data more clearly and identify potential LH surge patterns and the predicted time of ovulation within cycle variability.
Key Takeaways
- Polycystic ovary syndrome is often associated with irregular ovulation, which may make specialized tracking more relevant when planning for conception.
- An ovulation tracking app for PCOS may help identify individual hormone patterns that standard calendar-based apps may not always capture.
- Consistent tracking over 3 to 6 months may improve understanding of cycle trends and potential fertile windows.
- PCOS management through lifestyle changes and ongoing data monitoring may support better long-term reproductive health understanding.
- Combining ovulation test strips with app-based tracking may help provide a more complete view of hormone patterns than using a period tracker alone.
Key Terms Explained
- LH Surge: A rise in luteinizing hormone that typically signals the body might release an egg within about 24–36 hours.
- Anovulation: A cycle where an egg is not released, which is a common symptom in PCOS.
- Quantitative OPK: An ovulation test that provides a numerical LH value to help identify an LH peak and track hormone changes over time.
- Irregular Cycle: A menstrual cycle that varies in length or falls outside the typical range of 21 to 35 days, a pattern often observed in conditions like polycystic ovary syndrome and associated with hormonal variation.
- Basal Body Temperature (BBT): The body’s lowest resting temperature, which may shift upward after ovulation.
What Is an Ovulation Tracking App for PCOS, and How Does It Work?
An ovulation tracking app for PCOS may be described as a tool designed to help interpret hormonal patterns in individuals with irregular cycles. Unlike standard period trackers that often rely on calendar-based predictions, a PCOS-focused system may use biological inputs such as LH levels, symptoms, and cycle data to build a more personalized view of the cycle. According to NCBI, tracking these markers over time may help improve awareness of cycle patterns and potential predictability in certain individuals.
How Hormone Tracking for PCOS Improves Fertility
Hormone tracking for PCOS may help users understand their individual baseline LH levels. This may be relevant because some individuals with PCOS tend to have relatively elevated LH levels throughout the cycle, which could make standard ovulation tests more complex to interpret.
Why Regular Period Tracker Apps Often Fail for Tracking PCOS
Many standard apps are based on an assumed 28-day cycle with ovulation around day 14. For individuals with irregular cycles, these assumptions may not align with actual patterns, which could lead to less accurate fertile window estimates and potential confusion.
PCOS Tracking App vs Standard Period Tracker: What’s the Difference?
Standard period tracker apps often rely on calendar-based predictions, assuming a consistent cycle length and ovulation timing. PCOS-focused tracking may instead use biological signals such as LH levels, temperature, and symptoms to help identify patterns over time, which may be more relevant for irregular cycles.
- Standard period tracking — estimate based on calendar
- PCOS tracking — tracks hormone patterns and variability
Why Tracking Ovulation Is Hard With PCOS
Tracking ovulation with PCOS may be more challenging due to hormonal variation associated with the condition. Elevated androgen (male hormones like testosterone) levels may interfere with normal follicle development, which could delay ovulation or result in cycles where ovulation may not occur.
Irregular Cycles and Delayed Ovulation
In individuals with polycystic ovary patterns, ovulation may occur later than expected in the cycle — sometimes extending beyond day 30 or even day 40 — or may not be observed in some cycles. This variability may make timing intercourse based only on calendar estimates less reliable, and additional tracking methods may provide more clarity.
Multiple LH Surges in PCOS
The body may show more than one rise in luteinizing hormone within a single cycle. These patterns may appear as multiple peaks on ovulation tests, where LH increases without immediate ovulation, followed by a later rise that may be more closely associated with ovulation timing.
To understand which peak may be the true ovulatory peak, tracking BBT and PdG alongside OPKs may be helpful. A sustained rise in basal body temperature of about 0.5–1.0°F after one of the LH peaks may suggest that ovulation has likely occurred. In addition, PdG levels rising to around ≥5 ng/mL in the days following a peak may indicate progesterone activity, which is typically associated with the post-ovulation phase. Using these markers together may help differentiate between multiple LH surges and identify the peak that is more closely linked to ovulation.
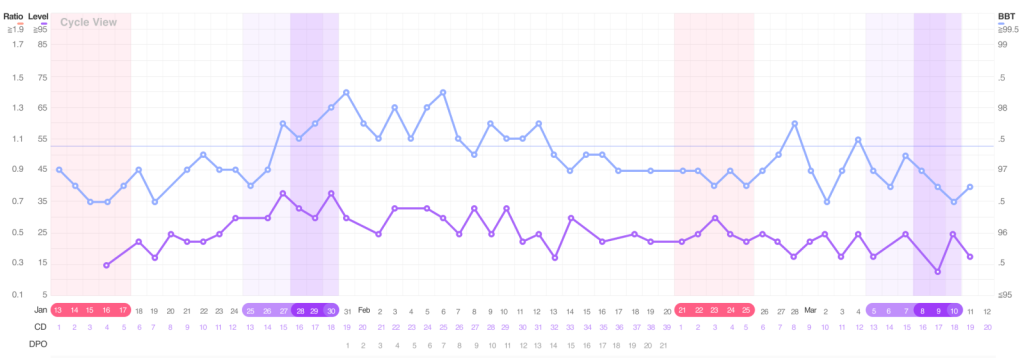
6-Month PCOS Fertility Tracking Plan (Step-by-Step)
Because PCOS cycles may be unpredictable, tracking over a longer period of time may be more helpful than relying on a single cycle. Following a structured PCOS tracking approach may help build a more complete dataset over time, which may improve understanding of cycle patterns and potential fertile windows.
Step-by-Step Guide to Tracking Your Fertility
Step 1: Begin OPK Testing After Your Period Ends
Test daily using easy@Home ovulation strips, ideally between 10 AM and 8 PM. In some cases, testing twice a day may help capture shorter LH surges. Continue testing each day until you observe your LH peak (when the test line becomes as dark as or darker than the control line), and for an additional 1–2 days after the peak to confirm the surge pattern. If you’re unsure about the best time of day to test, our guide on when to take an ovulation test can help you optimize your timing.
Step 2: Log Results in the Premom Ovulation Tracking App
Upload your test strips to view numerical LH values and visualize your hormone trends over time, which may help you identify patterns instead of relying on a single result.
Step 3: Identify Your Personal LH Peak
With PCOS, focus on your highest relative rise compared to your baseline rather than just a dark line. To find your true peak, pair OPKs with BBT and PdG. A sustained BBT rise (about 0.5–1.0°F or 0.3–0.5°C) and PdG levels around ≥5 ng/mL after a high LH peak may suggest that ovulation has likely occurred at that time.
Step 4: Pair With BBT Tracking
Measure your basal body temperature each morning. A sustained rise of about 0.5 to 1.0°F, 2–4 days post LH peak, may suggest that ovulation has likely occurred. If you’re new to temperature tracking, you can learn how to track basal body temperature for ovulation in our step-by-step guide.
Step 5: Look for Patterns Across Cycles
Over 2 to 3 cycles, observe whether LH peaks become more consistent or easier to identify. These trends may indicate changes in how your cycle is functioning, though responses can vary between individuals.
Step 6: Track PdG After the LH Peak
After you notice an LH peak and a possible BBT rise, PdG (progesterone metabolite) test strips can provide additional context. Testing in the days following ovulation may help indicate whether progesterone levels are rising. A positive PdG result over consecutive days may suggest that ovulation has likely occurred, though it should be interpreted alongside other signs.
Following these steps consistently for about 6 months may help build a clearer picture of your cycle patterns. Over time, this approach may make it easier to recognize recurring LH trends, temperature shifts, and progesterone patterns, which may support more informed fertility planning.
To track these signals together more easily, the Premom ovulation tracking app works alongside easy@Home ovulation test strips to track LH patterns, basal body temperature (BBT), PdG results, and symptoms in one place. This combined approach may be especially helpful for individuals with PCOS or irregular cycles, where hormone patterns may vary from cycle to cycle.
Why Premom’s PCOS Pro Works Better
While the standard Premom app focuses on tracking cycle data and estimating fertile windows, PCOS Pro may place more emphasis on interpreting irregular hormone patterns over time. This approach may be especially relevant for individuals with PCOS or unpredictable cycles, where single-cycle predictions may not always reflect underlying patterns.
PCOS Pro is a 6-month access pass within the Premom app, designed for individuals with irregular cycles or PCOS. It provides access to additional tools and resources that may support deeper cycle awareness.
What PCOS Pro may include:
- Tracking tools tailored for irregular or variable cycles
- Daily health logs for sleep, nutrition, and stress patterns
- Cycle insights that may become more informative as more data is collected
- Educational content focused on PCOS and hormone health
By combining these signals over time, users may gain a clearer understanding of their individual cycle patterns rather than relying on single data points.
Can You Get Pregnant With PCOS Using Tracking?
Getting pregnant with PCOS may be possible when the timing of ovulation is better understood and tracked. According to the WHO, PCOS may affect roughly 1 in 10 women of childbearing age. Some individuals may find improved outcomes through consistent monitoring and awareness of their cycle patterns.
How Tracking May Support Your Chances of Getting Pregnant
Tracking irregular cycles may help couples better understand when ovulation might happen and time intercourse during the fertile window. This may support the chances of fertilization, since the egg can only be fertilized for a short time after ovulation.
PCOS Self-Care + Tracking for Better Results
PCOS self-care may include lifestyle habits that support the patterns seen in your fertility tracker. When tracking is combined with daily routines, it may help you better understand how your cycle responds over time.
Nutrition Tracking for PCOS
A healthy diet for polycystic ovary syndrome, when combined with a fertility tracker, may support a better understanding of cycle patterns. A nutrition approach for PCOS often focuses on insulin balance, as insulin and androgens may be connected. Balanced meals with protein, fibre, and healthy fats may support more stable hormone patterns in some individuals.
Lifestyle and Insulin Resistance
Sleep, stress, and physical activity may influence hormonal patterns. Consistent sleep and moderate exercise may support overall balance, while higher stress levels may be associated with delayed ovulation in some cases. Tracking these factors along with ovulation signs may provide a clearer picture of your cycle over time. Some individuals also explore targeted supplements as part of their routine — you can learn more about commonly used PCOS supplements for fertility in our detailed guide.
Frequently Asked Questions (FAQs)
Yes, the Premom app may allow users to log PCOS-related symptoms such as acne, hair growth, and pelvic discomfort alongside their cycle data.
In addition, the app includes a PCOS self-assessment feature that shows how your responses compare to commonly reported PCOS patterns. This assessment may help identify patterns related to irregular cycles or hormonal imbalance and guide users on the next steps for fertility planning.
Ovulation may be harder to track in PCOS because hormone levels can fluctuate, and cycles may not follow a predictable pattern, which can make standard calendar-based predictions less reliable.
A system that includes quantitative LH testing and app-based analysis, such as easy@Home with Premom, may be helpful for individuals with irregular cycles, as it may provide more detailed insights, such as LH trend patterns, identification of multiple peaks, understanding personal baseline levels, and the ability to correlate hormone changes with symptoms and cycle variability over time, which may not be possible with calendar-based tracking alone.
A PCOS self-assessment, such as the one found in the Premom App, or online screening tool may help identify patterns. However, a clinical diagnosis may require evaluation by a doctor, including assessment of hormone levels, menstrual history, and ovarian appearance.
The app uses algorithm-based analysis to interpret LH trends across cycles, which may help users review multiple LH rises and identify patterns that could be difficult to interpret with basic tracking methods. It also allows tracking of basal body temperature (BBT) and PdG levels, which may provide additional context for understanding possible ovulation patterns. Combining these signals may offer a more complete view of cycle variability in PCOS.
Fertility predictions may become more informative after collecting data over a few cycles. Tracking LH trends, basal body temperature (BBT), PdG levels, cycle length, cervical mucus, and symptoms over time may help improve understanding of individual hormone patterns and cycle variability, especially in PCOS.
In many cases, tracking consistently for 2 to 3 cycles or longer may help reveal patterns, although this can vary depending on cycle irregularity.
Disclaimer: Premom provides educational information and tracking tools. It is not medical advice. For medical guidance, consult a healthcare professional. Premom’s Ask AI is purely informational and educational and is not a substitute for professional medical advice, diagnosis, or treatment of any kind.
References
- Teede HJ, Misso ML, Costello MF, et al. Recommendations from the international evidence-based guideline for the assessment and management of polycystic ovary syndrome. Fertil Steril. 2018;110(3):364–379. Available here
- McCartney CR, Marshall JC. Polycystic Ovary Syndrome. N Engl J Med. 2016;375(1):54–64. doi:10.1056/NEJMcp1514916 Available here
- World Health Organization. Polycystic ovary syndrome (PCOS). 2026. Available here
- Johnson SR, Godbert S, Perry P, et al. Accuracy of a home-based device for giving an early estimate of pregnancy duration compared with reference methods. Fertil Steril. 2013;100(6):1635–41. doi:10.1016/j.fertnstert.2013.08.031 Available here