You’re Not Alone! If you are pregnant, or trying to conceive (TTC), and you just received a lab result sheet with the words “Low Progesterone” highlighted, you are likely feeling a wave of concern and questions.
It is absolutely normal to immediately jump to conclusions:
- “Did my body fail this pregnancy?”
- “Does this mean I’ll never be able to carry a baby?”
First, take a deep breath. We understand your fear, especially if you have a history of loss or lengthy fertility struggles. That piece of paper with a number on it can feel like a disappointing verdict.
But here is the most important reassurance: Many people do go on to have healthy, successful pregnancies, even with low progesterone results.
Progesterone is a vital hormone, but it is not a simple “pass/fail” test. Its levels are complex, constantly fluctuating, and often just one small piece of a much larger, and often hopeful, puzzle.
Pregnancy with Low Progesterone – Key Takeaways
- Crucial but Fluctuating: Progesterone is vital for maintaining the uterine lining, though levels naturally vary throughout the day.
- Not a Definitive Sign: Low levels don’t always mean a pregnancy will fail; many go on to be healthy with proper monitoring.
- Supportive Supplementation: Bio-identical Progesterone medication can easily bridge the gap until the placenta takes over hormone production around weeks 10-12.
- Focus on Trends: Doctors prioritize long-term hormone trends over single test results to assess pregnancy health.
What Progesterone Does in Early Pregnancy
Progesterone is one of the most important hormones in the reproductive system. It is often called the “hormone of pregnancy” for a very good reason.
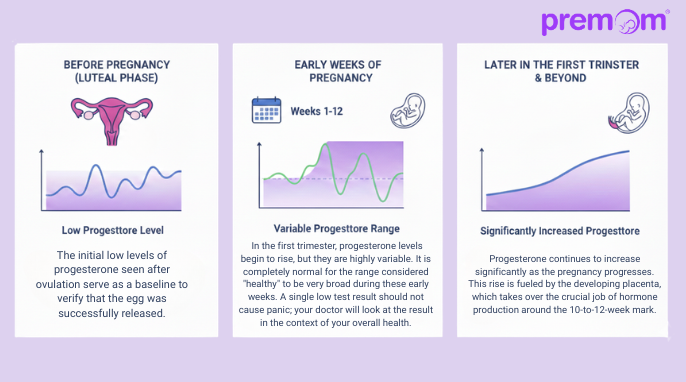
Progesterone’s Role in the First Trimester
After ovulation, the release of an egg, the remaining shell of the follicle turns into a temporary structure called the corpus luteum. This corpus luteum immediately starts producing large amounts of progesterone.
In early pregnancy, progesterone is responsible for three critical jobs:
- Supports the Uterine Lining (Endometrium): Progesterone transforms the uterine lining (the endometrium) from thick and proliferative to spongy, receptive, and nutrient-rich. This creates the perfect, soft environment for the fertilized egg to implant.
- Reduces Uterine Contractions: It acts as a smooth muscle relaxant, preventing the uterus from contracting and potentially expelling the developing embryo.
- Aids Early Placental Development: Progesterone helps support the early development of the placenta, the organ that will eventually take over hormone production and sustain the entire pregnancy.
Without adequate progesterone, the uterine lining may not be maintained, leading to early spotting or failure of implantation.
Why Progesterone Levels Vary So Much
Understanding progesterone’s normal fluctuations is key to reducing anxiety. It is not a hormone that stays steady all day; it is pulsatile, meaning it is released in short, intense bursts every few hours.
- Natural Daily Fluctuations: A progesterone blood test taken at 8:00 AM might look significantly lower than one taken at 2:00 PM on the same day and vice versa.
- Timing of Tests: The number will also vary drastically depending on where you are in your cycle (luteal phase versus early pregnancy) and whether the test is measuring the hormone in the bloodstream (serum) or the urine metabolite (PdG).
Because of this natural, constant variability, progesterone is important, but it is not a single “pass/fail” hormone. Doctors almost always look at trends (multiple tests over several days) rather than judging an entire pregnancy on one isolated number.
Understanding Progesterone Numbers
The moment you see your lab results, your brain demands to know: “What is a good number?” Unfortunately, there is no single, magic number.
Understanding your progesterone numbers can be confusing because the required levels change dramatically throughout your cycle and pregnancy.
Because every lab uses different measuring standards and every individual’s hormone pulse is unique, you should always refer to the specific “normal” reference range provided by your testing laboratory and discuss your individual results directly with your doctor. They are best equipped to interpret the result alongside your symptoms and other blood work (like hCG).
The exact number your doctor hopes to see varies widely by how far along you are in the pregnancy.
“My Progestreone Level Was 12 — Is That Bad?”
The most commonly cited thresholds you see online are 10, 12, or 15 nanograms per milliliter (ng/mL) to sustain a healthy pregnancy. Many doctors feel comfortable with a baseline above 10 ng/mL in early pregnancy, but even this isn’t a hard rule.
What doctors actually consider concerning is not the single number, but the trend.
Some concerning findings may include:
- A progesterone level that drops steadily over several days.
- A low progesterone level combined with stagnant or dropping hCG levels.
- Low progesterone combined with worrisome symptoms like heavy bleeding or significant cramping.
If your single blood draw was 12 ng/mL, but your hCG is rising beautifully and your scan looks good, your doctor is much less likely to be worried than if your level was 15 ng/mL but your hCG was declining. The complete picture is always what matters.
Low Progesterone & Miscarriage
It is absolutely crucial to understand the nuance in the relationship between low progesterone and pregnancy loss.
For many years, it was debated whether low progesterone was the cause of a miscarriage or simply a signal of one. Current research suggests it is often the latter.
When a pregnancy is not genetically viable (meaning there is a chromosomal issue with the embryo), the body senses this. The hormonal signals necessary to maintain the corpus luteum (like hCG) fade, and the progesterone production naturally shuts down.
In this scenario:
- Low progesterone is a signal, not the cause. It is a response by the body to a non-viable pregnancy.
- Taking progesterone supplements in this case won’t prevent the miscarriage, but it may artificially delay it.
The good news is that for many people, the low number is simply due to poor luteal function or bad timing of the blood draw or if it is a low progesterone, prescription progesterone is easily available and has a high safety profile. In these cases, treatment can be highly effective.
Can You Get Pregnant With Low Progesterone?
Short Answer — Yes, It’s Possible
The fear that low progesterone makes pregnancy impossible is valid, but it is simply not true. Many successful pregnancies proceed despite low or borderline initial levels, often with the support of supplementation.
Success stories are built on:
- Early Detection + Supplementation: Catching a low level early and beginning support immediately.
- Stable or Rising hCG: This is the most important piece of data, indicating the embryo is growing.
- Close Monitoring: Consistent blood draws and scans to track the progression.
When Low Progesterone Is More Concerning
Low progesterone results merit closer scrutiny if you have:
- Recurrent Pregnancy Loss (RPL) History: If you’ve experienced multiple losses, your doctor will be more proactive about starting support.
- Spotting + Dropping Levels: This combination strongly indicates the uterine lining is breaking down.
- Known Luteal Phase Defect (LPD): A short luteal phase (the time between ovulation and your period) or consistently low progesterone after ovulation.
- Assisted Reproductive Cycles (IVF/IUI): In IVF, progesterone is mandatory because the retrieval process removes the corpus luteum.
Real-World Success Stories
While every person’s body is unique, successful outcomes with low progesterone often share common data patterns:
- The initial low progesterone level quickly stabilized or rose after starting supplemental medication.
- The hCG levels (the pregnancy hormone) showed the necessary doubling time (About every 48 hours).
- Early ultrasounds confirmed the pregnancy was properly implanted in the uterus (not ectopic) and, eventually, a fetal heartbeat was detected.
These patterns emphasize data trends over isolated values.
Low Progesterone Symptoms
When you are feeling anxious, every ache and twinge can be magnified into a sign of trouble. It is important to separate reliable symptoms from normal pregnancy discomfort.
Commonly Reported Symptoms
Low progesterone symptoms that may include:
- Spotting or light bleeding: This is the primary physical sign that the uterine lining may not be maintained.
- Cramping: Mild cramping is normal as the uterus grows, but severe, persistent, or cyclical cramping should be reported to your doctor immediately.
Anxiety can be amplified by symptom-watching: When you are looking for symptoms, you are more likely to find and fixate on them. If you experience any bleeding or moderate to severe cramping in pregnancy, always consult your healthcare provider immediately.
Symptoms That Are Not Reliable Progesterone Indicators
These common pregnancy signs are controlled by other factors (like hCG) and are not reliable indicators of your progesterone level:
- Breast tenderness
- Fatigue
- Nausea (or lack of it)
This is a time of immense emotional volatility. Be gentle with yourself, but always rely on your doctor’s orders and lab results.
Why Progesterone Can Be Low
It is crucial to release the self-blame. Low progesterone is nearly always a result of a physiological process, not something you did or didn’t do.
Ovulation Quality & Corpus Luteum Function
The single biggest reason for low progesterone is poor function of the corpus luteum (the structure that makes progesterone after the egg is released). This can be caused by:
- Late Ovulation: An egg released late in the cycle may result in a weaker corpus luteum.
- Short Luteal Phase: If the corpus luteum only survives for 10 days or less, it may not produce enough progesterone to sustain the lining until the placenta can take over.
- Stress-Related Hormonal Disruption: Extreme physical or emotional stress can interfere with the signals the brain sends to the ovaries, impacting ovulation quality.
Medical & Cycle-Related Causes
Underlying conditions can also impact progesterone production:
- PCOS (Polycystic Ovary Syndrome): Hormonal imbalances can impact the follicle’s ability to release a quality egg.
- Thyroid Imbalance: An overactive or underactive thyroid can disrupt the complex balance of reproductive hormones.
- Endometriosis: This condition can create an inflammatory environment that interferes with egg quality and luteal function.
- Age-Related Hormonal Shifts (especially 35+): As ovarian reserve declines, the quality of the ovulated egg and the resulting corpus luteum can sometimes be affected.
After Pregnancy Loss, Why Progesterone Gets Extra Scrutiny
If you are monitoring progesterone after a loss, it is often due to trauma-driven monitoring. When a prior loss has no clear cause, progesterone becomes a common factor to check, sometimes leading to retrospective blame. Your current care should be forward-looking, not focused on assigning blame to past events.
Progesterone Supplementation — Does It Actually Help?
The answer to this question depends entirely on the cause of the low progesterone. If the low level is due to poor corpus luteum function, supplementation can bridge the gap until the placenta develops.
Types of Progesterone Support
Progesterone supplements are often referred to as Progesterone Replacement Therapy (PRT) or Luteal Phase Support (LPS).
- Vaginal Suppositories: The most common and often preferred method. They are inserted directly into the vagina and deliver progesterone right to the uterus with fewer systemic side effects.
- Oral Progesterone: Pills taken by mouth. Less efficient for uterine delivery but can be easier for some to manage.
- Injectable Progesterone (PIO): Progesterone-in-Oil shots, typically used for IVF cycles where a higher, controlled dose is required. These can be painful but highly effective.
- Sublingual compounded progesterone in sublingual ‘troches’ are also sometimes used as well as progesterone creams that are absorbed through the skin.
Are Progesterone Suppositories Safe for the Baby?
Yes. Progesterone supplements (suppositories, injections, or oral) are routinely prescribed in early pregnancy and have been used for decades. The vast majority of research finds them safe and does not indicate any risk of birth defects. They are commonly prescribed because they have the potential to help maintain the pregnancy when the body’s natural production is insufficient.
Who Benefits Most From Supplementation
Research has shown the greatest benefit for progesterone supplementation in two groups:
- Women with a history of three or more recurrent pregnancy losses (RPL).
- Women undergoing Assisted Reproductive Technology (ART) like IVF.
It is also commonly prescribed for those with early spotting and low progesterone, even without a history of RPL, as a supportive measure.
How Long Do You Usually Take Progesterone?
The typical timeline is until 12-15 weeks of gestation. This is because, at this point, the growing placenta is large and mature enough to take over the primary production of progesterone, rendering the supplemental dose unnecessary. Your doctor will then guide you on slowly tapering off the medication; stopping abruptly is generally not advised.
Monitoring Progesterone Without Losing Your Mind
Tracking fertility data is powerful, but it can quickly become an anxiety-inducer if not approached correctly.
Blood Tests vs PdG (Urine Metabolite) Testing
When talking about progesterone testing, you will likely hear about two different methods, each with its own benefits and limitations:
- Blood Serum Test: This is the traditional test done at your doctor’s office or a lab. It measures the actual concentration of progesterone in your blood at the exact moment the blood is drawn.
- Pros: This is the gold standard used by doctors to officially confirm pregnancy health and guide treatment, especially when prescribing supplements.
- Limitations: Because progesterone is released in bursts (it’s highly pulsatile), the number only reflects a single moment in time. This is why a single low draw might not show the whole picture. It also requires a trip to the lab or clinic.
- PdG (Urine Metabolite) Testing: This test, often done at home with test strips, measures Pregnanediol-3-Glucuronide (PdG), which is the inactive breakdown product of progesterone found in your urine.
- Pros: PdG tests are non-invasive and affordable, allowing you to test at home every day. Since PdG levels reflect the body’s progesterone production over the last 24 hours, they are excellent for showing the average trend of your hormone.
- Limitations: PdG does not measure the exact concentration of progesterone in the blood, and it generally cannot be used to monitor the effectiveness of prescribed progesterone supplements.
Your doctor uses the blood test for clinical decisions, while home PdG tests are a powerful tool for you to establish your baseline, track ovulation and patterns over time.
How Tracking Reduces Anxiety (Instead of Increasing It)
The key is to look for patterns over time instead of looking at just a single result.
- Preconception: Tracking your PdG levels during the luteal phase (after ovulation) helps you establish your healthy baseline.
- Early Pregnancy: Monitoring your trend (multiple blood tests) gives your medical team actionable data to determine if your supplement dose is working or if the pregnancy is progressing normally. This empowers you, rather than just waiting in fear.
What to Do Right Now If You’ve Been Told Your Progesterone Is Low
Take action. Empower yourself with information and clear communication with your medical team.

What Not to Do
- Do not start or stop any supplement (especially progesterone) without explicit medical advice.
- Do not enforce bed rest unless specifically advised by your doctor.
- Do not self-blame or compare your numbers to strangers online. Their history, lab, and testing timing are all different from yours.
- Do not fall for the myth of miracle foods. While nutrition is key, you cannot overcome a major hormonal deficiency with diet alone. However, focusing on nutritional support is always good for overall health. [Foods To Naturally Increase Progesterone]
Gentle Self-Care While You Wait
This period of waiting can be emotionally draining. Focus on gentle, immediate self-care:
- Emotional Regulation Strategies: Allow yourself to feel the fear, but try to limit “reassurance-seeking spirals” (endlessly Googling or testing). Set a timer for 15 minutes of worry, and then put your phone down.
- Allow Cautious Hope: Focus on the fact that your body has achieved a pregnancy. You are receiving monitoring and care. Hope is a vital ingredient, and you are allowed to hold onto it.
Understanding Progesterone
Your low progesterone result is a piece of data, not a complete sentence and the hope for a healthy pregnancy is absolutely real.
By working closely with your doctor, utilizing the right supplemental support when necessary, and prioritizing your mental health, you are doing everything you can to create the best possible outcome. Understanding your progesterone numbers and the nuances of supplementation is a powerful way to manage anxiety and take charge of your care.
Ready to dive deeper into your cycle? Download the Premom app to start tracking your ovulation and progesterone metabolite (PdG) trends today. Understanding your body is the first, most powerful step in this journey.
Frequently Asked Questions about Pregnancy and Low Progesterone
Immediately contact your healthcare provider. They will likely order a second blood test (often with an hCG draw) to establish a trend. Based on your symptoms and history, they may recommend starting prescription progesterone supplements (vaginal suppositories or oral tablets).
There is no single “too low” number, but a level consistently below 10 ng/mL in the first 5-6 weeks of pregnancy is considered suboptimal and is often a signal for intervention. More important than the single number is a dropping trend over multiple tests.
Low progesterone can signal a miscarriage (because the hormone drops in response to a non-viable pregnancy) or it can be a contributing cause if your corpus luteum is weak and fails to maintain the uterine lining. This distinction is often impossible to make, but treatment aims to support the pregnancy when corpus luteum failure is suspected.
Progesterone supplementation can help to prevent miscarriage in cases only where the loss is caused by poor corpus luteum function or a documented luteal phase defect. They are particularly beneficial for women with a history of recurrent pregnancy loss (RPL) or those undergoing IVF. They will not prevent a miscarriage caused by a severe chromosomal abnormality in the embryo.
Common side effects include fatigue, dizziness, nausea, and headache. Vaginal suppositories may cause localized irritation or discharge. These are generally mild and cease once the medication is stopped around 12 weeks.
No. While spotting and cramping can be symptoms of low progesterone, they are not reliable indicators because they can be caused by many other factors. The only way to confirm low progesterone is through a blood test with your medical provider.
Resources:
Bataa M, Abdelmessih E, Hanna F. Exploring Progesterone Deficiency in First-Trimester Miscarriage and the Impact of Hormone Therapy on Foetal Development: A Scoping Review. Children (Basel). 2024 Apr 2;11(4):422. doi: 10.3390/children11040422. PMID: 38671639; PMCID: PMC11049201.
Ren Z, Sun X, Li Z, Yang H. Vaginal Bleeding After Pregnancy: Progesterone Levels and Pregnancy Outcomes in the First Trimester. Matern Fetal Med. 2025 Oct;7(4):256-257. doi: 10.1097/FM9.0000000000000285. Epub 2025 May 14. PMID: 41158426; PMCID: PMC12558237.
Micronized vaginal progesterone to prevent miscarriage: a critical evaluation of randomized evidence, Coomarasamy, Arri et al. American Journal of Obstetrics & Gynecology, Volume 223, Issue 2, 167 – 176
Haas DM, Hathaway TJ, Ramsey PS. Progestogen for preventing miscarriage in women with recurrent miscarriage of unclear etiology. Cochrane Database Syst Rev. 2018 Oct 8;10(10):CD003511. doi: 10.1002/14651858.CD003511.pub4. Update in: Cochrane Database Syst Rev. 2019 Nov 20;2019(11). doi: 10.1002/14651858.CD003511.pub5. PMID: 30298541; PMCID: PMC6516817.



