If you have been meticulously tracking your cycle, timing intercourse around ovulation, and still seeing a negative test month after month, you might be feeling a specific kind of exhausted frustration. You’re doing everything right. And yet your period keeps arriving earlier than it should.
That early arrival could be a clue. If the gap between ovulation and your period feels cramped, you might be dealing with a Luteal Phase Defect (LPD). Think of the luteal phase as the critical incubation window of your cycle. It’s when your body prepares the uterine lining for a fertilized egg to settle in. If that window closes too soon, pregnancy doesn’t have time to take hold.
This article covers how to recognize the key symptoms, what causes them, and how tracking tools like the Premom app can help you build a clear picture of your cycle before your next doctor’s appointment. If you’ve already been diagnosed and are wondering what to do next, our dedicated guide on getting pregnant with a short luteal phase covers treatment and management options in depth.
Key Takeaways
- A luteal phase shorter than 10 days can prevent an embryo from successfully implanting in the uterine lining
- Premenstrual spotting is one of the most common and overlooked Luteal Phase Defect symptoms
- Tracking basal body temperature (BBT) and testing progesterone levels are the most practical ways to identify a short luteal phase at home
- LPD is often caused by weak ovulation, thyroid disorders, insufficient progesterone levels, or chronic stress
What is the Luteal Phase and Why Does It Matter?
The luteal phase is the second half of your menstrual cycle. It begins the day after ovulation and ends the day before your next period. During this window, your body shifts focus from releasing an egg to sustaining an embryo.
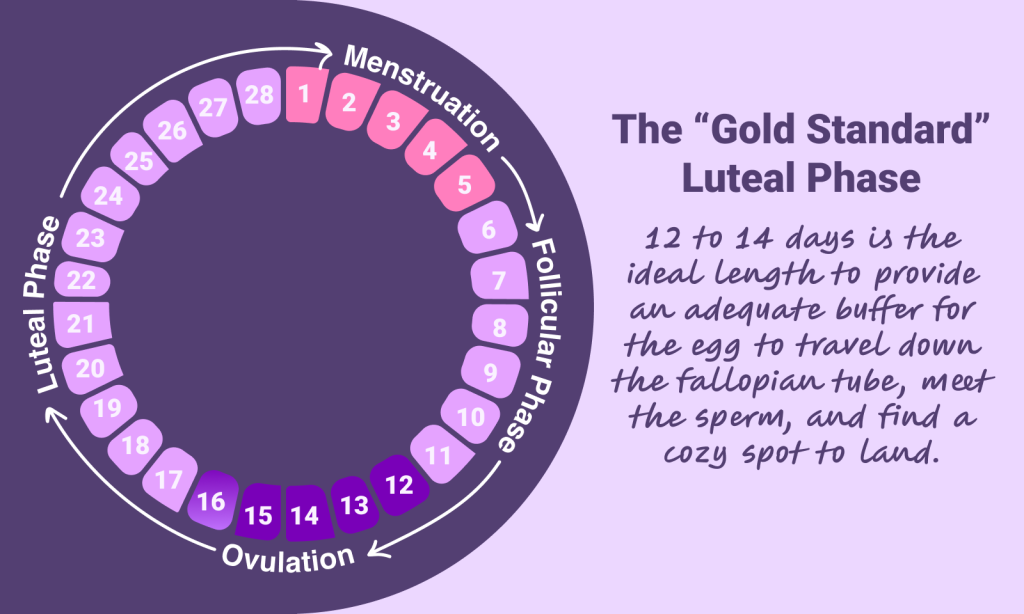
After ovulation, the follicle transforms into a temporary gland called the corpus luteum. This gland produces progesterone, which thickens the uterine lining and keeps it stable enough for implantation. A healthy luteal phase typically runs 12 to 14 days. Anything between 11 and 17 days is generally considered within normal range. Consistently shorter than 10 days is where problems begin.
As noted in Fertility and Sterility, the window of implantation typically occurs between days 6 and 10 after ovulation. If your period starts on day 8 or 9, the biological clock has run out before a pregnancy could begin.
Note: Clinical definitions of LPD continue to evolve. The American Society for Reproductive Medicine noted in 2021 that LPD is not always easy to diagnose through standard clinical testing alone, which is exactly why consistent cycle tracking becomes so valuable for building a case with your provider.
Common Questions About Luteal Phase Defect
How long is the luteal phase?
The luteal phase typically lasts 11 to 17 days, with 12 to 14 days considered ideal for conception. Unlike the first half of your cycle, which can shift based on stress or illness, the luteal phase length tends to stay consistent for each person month to month.
What is a luteal phase defect?
A luteal phase defect is when the second half of your menstrual cycle is consistently shorter than 10 days. This leaves insufficient time for a fertilized egg to implant before the uterine lining begins to shed. It is often linked to low or rapidly declining progesterone levels after ovulation.
Can a short luteal phase cause a miscarriage?
It can contribute to very early pregnancy loss. When the uterine lining starts to break down before an embryo has time to fully attach, the pregnancy cannot be sustained. Many women with LPD experience what appears to be a late period rather than a recognized pregnancy loss.
How do I know if my luteal phase is too short?
The most accessible way is to track your cycle over 2 to 3 months. Logging your basal body temperature daily creates a visible record of your thermal shift after ovulation, and counting days from that shift to your period start gives you your luteal phase length. The Premom app does this automatically when paired with an Easy@Home Smart Basal Thermometer.
Recognizing Key Luteal Phase Defect Symptoms
LPD can be easy to miss because it doesn’t necessarily stop you from ovulating. You might still get a peak reading on your OPK, which adds to the confusion. But your body often sends quiet signals that the second half of your cycle isn’t functioning as it should.
Physical Signs in Your Cycle
- Premenstrual spotting: Light pink or brown spotting 3 to 4 days before your full period begins is often the first red flag. It suggests progesterone is dropping prematurely, destabilizing the uterine lining before it should.
- Short overall cycles: If your entire cycle consistently runs under 24 days, your luteal phase is likely being cut short.
- A slow rise in BBT: After ovulation, basal body temperature should jump and hold. A gradual creep upward instead of a clear shift may indicate a struggling corpus luteum.
Emotional and Hormonal Indicators
Progesterone has a natural calming effect on the nervous system. When levels drop too fast or stay too low, the impact isn’t just physical. Women with LPD often describe heightened anxiety, poor sleep, pronounced mood swings, or a noticeable energy crash in the week before their period. These symptoms are real, and they’re worth logging alongside your cycle data.
Healthy Luteal Phase vs. Luteal Phase Defect

Understanding Common Luteal Phase Defect Causes
LPD is rarely an isolated issue. It’s usually a downstream signal from something else happening in your hormonal system.
Weak Ovulation
A strong luteal phase starts with a strong ovulation. If the follicle doesn’t develop robustly before releasing the egg, the resulting corpus luteum will be underpowered as well. Research published in The Journal of Clinical Endocrinology and Metabolism identifies inadequate follicular development as a primary driver of low progesterone secretion after ovulation. Simply put: if the launch isn’t strong, the landing won’t be either.
Underlying Health Conditions
- Thyroid disorders: Both hypothyroidism and hyperthyroidism can interfere with progesterone production and cycle regularity.
- PCOS: Polycystic Ovary Syndrome often involves irregular or incomplete ovulation, which can leave the corpus luteum underdeveloped.
- Chronic stress and the progesterone steal: Under sustained stress, your body prioritizes cortisol production. Because cortisol and progesterone share the same hormonal building blocks, high cortisol effectively competes with progesterone for resources. Your body, in survival mode, will choose cortisol every time.
How to Identify LPD Using the Premom App and Testing
The hardest part of suspecting LPD is the guessing. You notice spotting or a short cycle, but without data, there’s nothing concrete to bring to a doctor. Building a cycle map over 2 to 3 months changes that.
Tracking BBT with the Premom App
Basal body temperature is a direct window into progesterone activity. After ovulation, your resting temperature should rise and hold. When you sync an Easy@Home Smart Basal Thermometer with the Premom app, your temperatures are logged automatically each morning. The app marks your thermal shift and counts the days from that shift to your period start, giving you a clear luteal phase length without any manual math.
If the app consistently shows 9 days between your thermal shift and your period, that’s useful data your healthcare provider can act on. It moves the conversation from “I think my luteal phases are short” to “here are three months of charts that show it.”
Verifying Progesterone with PdG Testing
OPKs tell you when your body is building toward ovulation. They can’t tell you whether ovulation was strong enough to sustain a pregnancy. That’s a different question, and it requires a different tool.
PdG (progesterone metabolite) test strips measure a urine-based marker of progesterone in the days after ovulation. Testing with Easy@Home PdG strips during your luteal phase and logging results in the Premom app lets you see both whether ovulation likely occurred and how your progesterone levels trend over time. If levels look low or drop off quickly, that pattern becomes part of your tracking record.
Important: PdG testing supports your tracking picture. It does not diagnose a luteal phase defect or replace a blood progesterone test ordered by your provider.
Next Steps: Supporting Your Luteal Phase Health
A short luteal phase is frustrating, but it’s one of the more manageable cycle issues to address. For many women, targeted lifestyle changes make a measurable difference. And when they don’t, consistent tracking data means your provider can move quickly to the right intervention.
- Herbal support: Vitex (chaste tree berry) may support progesterone production and luteal phase function by gently influencing the hypothalamic-pituitary-ovarian axis.* When using a dry extract formulation), typical dosing ranges from 800–1,000 mg daily for at least 2–3 cycles to assess its impact on your cycles. While not a guaranteed fix, it’s a reasonable option to discuss with your provider alongside your tracking data.
- Stress management: Reducing cortisol load directly supports progesterone production. Consistent sleep, lower intensity exercise during the luteal phase, and stress reduction practices can all help interrupt the progesterone steal pattern.
- Medical consultation: If your Premom charts consistently show a luteal phase under 10 days, bring them to your doctor. Having 2 to 3 months of BBT data and PdG results gives your provider a far clearer starting point than a single blood draw. Prescription of bioidentical progesterone can be supportive for women with luteal phase defect caused by low progesterone levels.
Identifying a luteal phase defect is a meaningful step forward. Once you understand why the incubation window is falling short, you have something to work with. You’re not broken. Your body is asking for a little extra support.
Luteal Phase Defect Symptoms and Causes: FAQs
It’s possible, but more challenging. Implantation typically occurs between days 6 and 10 after ovulation. If your period starts on day 8 or 9, the uterine lining may begin to shed before the embryo has had time to firmly attach. Extending the phase, through lifestyle changes or medical support, is usually the first priority.
Pre-menstrual spotting is a classic indicator of a luteal phase issue. It usually means progesterone is dropping too early, causing the uterine lining to become unstable before a full period trigger. Rather than a sharp progesterone drop leading to a clean period start, the slow decline causes that light, early spotting first.
Not always, but the two are closely linked. You can have a luteal phase that looks normal in length but still have progesterone levels too low to sustain a pregnancy. This is why PdG testing matters: it gives you a view of the quality of your luteal phase, not just the length. Both pieces of data together tell a much more complete story.
Some research supports the use of Vitex (chaste tree berry) to help support progesterone production and luteal phase function. When using a dry extract formulation, it’s typically taken daily for 2–3 cycles to assess effectiveness. That said, supplements should complement a clear data picture — not replace one. Track for 2–3 cycles first, then discuss supplementation with your provider based on what your data shows.
Yes. The strength of your luteal phase depends directly on the strength of your ovulation. A follicle that doesn’t develop fully in the first half of your cycle will produce a weak corpus luteum with limited progesterone output. Tracking your LH surge in the Premom app helps you assess the strength of your ovulatory signal over multiple cycles.
It can. Chronic stress and excessive physical strain both elevate cortisol, which competes directly with progesterone production. If you notice your luteal phase shortening during particularly demanding months, that’s a signal worth taking seriously, not just a coincidence.
*These statements have not been evaluated by the U.S. Food and Drug Administration. This product is not intended to diagnose, treat, cure, or prevent any disease. The information provided is for educational purposes only and is not medical advice. Please consult your healthcare provider before starting any new supplement, especially if you are pregnant, nursing, taking medication, or have a medical condition.
References
Wilcox, A. J., Baird, D. D., & Weinberg, C. R. (1999). Time of implantation of the conceptus and loss of pregnancy. New England Journal of Medicine, 340(23), 1796-1799. https://doi.org/10.1056/NEJM199906103402304
Sherman, B. M., & Korenman, S. G. (1974). Measurement of serum LH, FSH, estradiol and progesterone in disorders of the human menstrual cycle: The inadequate luteal phase. The Journal of Clinical Endocrinology and Metabolism, 39(1), 145-149. https://doi.org/10.1210/jcem-39-1-145
Mesen TB, Young SL. Progesterone and the luteal phase: a requisite to reproduction. Obstet Gynecol Clin North Am. 2015 Mar;42(1):135-51. doi: 10.1016/j.ogc.2014.10.003. PMID: 25681845; PMCID: PMC4436586.
Henmi, H. et al. Effects of ascorbic acid supplementation on serum progesterone levels in patients with a luteal phase defect. Fertility and Sterility, Volume 80, Issue 2, 459-461.
Practice Committee of the American Society for Reproductive Medicine. (2021). Current clinical irrelevance of luteal phase deficiency: A committee opinion. Fertility and Sterility, 115(6), 1411-1416. https://doi.org/10.1016/j.fertnstert.2021.02.010
Van Die, M., Burger, H. G., Teede, H. J., & Bone, K. M. (2013).Vitex agnus-castus extracts for female reproductive disorders: A systematic review of clinical trials.Planta Medica, 79(6), 562–575. https://doi.org/10.1055/s-0032-1327831



